Modern restorative dentistry
Modern restorative dentistry integrates advanced technologies and biocompatible materials to deliver more precise and comfortable treatments. Options such as screwless dental implants offer a less invasive approach, shorter recovery times, and natural-looking results tailored to individual patient needs. These developments help simplify procedures while improving overall dental outcomes.
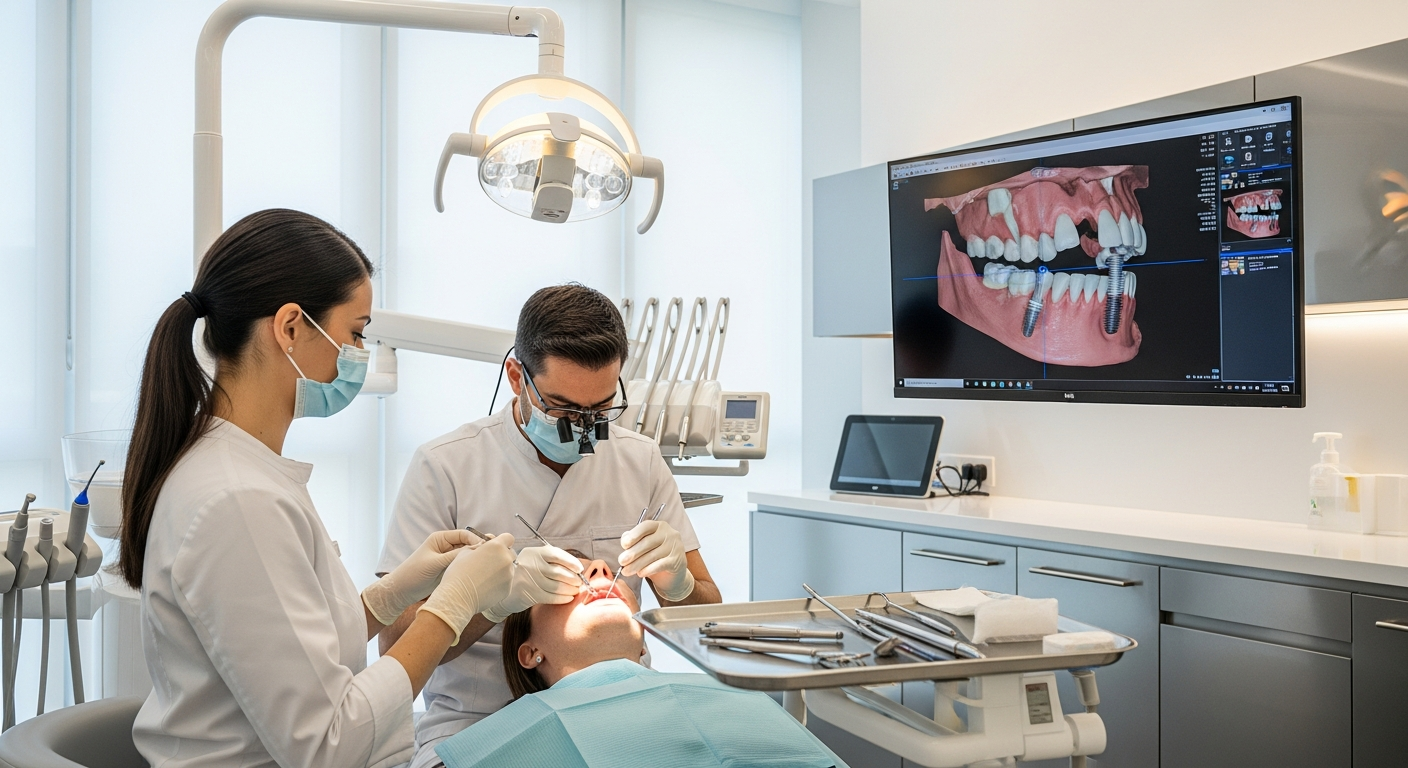
Replacing or repairing teeth is no longer limited to “one-size-fits-all” approaches. Many UK clinics now combine careful diagnosis, minimally disruptive techniques, and digitally planned restorations to improve fit and reduce uncertainty. For patients, that often translates into clearer treatment discussions, more predictable timelines, and a stronger focus on comfort during healing. The key is understanding how these tools and methods work together, and where their limits are.
How do screwless implants work today?
“Screwless” is often used to describe restorations that don’t rely on a visible screw access hole in the final tooth, or that use alternative retention methods for the crown. In practice, clinicians may use cement-retained crowns, friction-fit designs, or modern connection geometries intended to improve stability. The important distinction is not marketing language, but how the restoration is retrieved for maintenance, how excess cement is controlled, and how the bite forces are managed. Ask how the restoration would be removed if adjustments are needed, and how long-term cleaning and monitoring will be handled.
What makes modern dentistry less invasive?
Less invasive procedures in modern dentistry typically start with better planning and more conservative handling of soft tissue and bone. Where appropriate, clinicians may consider flapless or reduced-flap approaches, tissue-preserving incision designs, and targeted grafting strategies rather than broader surgical exposure. Not every case is suitable—bone volume, gum health, and infection risk still matter—but the overall trend is to minimise disruption while protecting long-term stability. A careful assessment (including medical history and oral health habits) is central, because “less invasive” should never mean “less thorough.”
Which digital tools improve restoration accuracy?
Digital technologies in dental restoration commonly include intraoral scanners, 3D imaging (such as CBCT where clinically justified), CAD/CAM design, and 3D-printed or milled guides and provisional teeth. Digital scans can reduce the need for traditional impressions and help capture bite relationships with greater clarity. When combined with planning software, clinicians can visualise the position of planned restorations relative to available bone and neighbouring teeth. However, accuracy still depends on clinical judgement, scan quality, and good communication with the dental laboratory. Digital workflows support decision-making; they do not replace it.
How can recovery be faster and more comfortable?
Faster recovery and improved patient comfort depend on both technique and aftercare. Shorter procedures, gentler tissue handling, and well-fitting temporary restorations can reduce irritation and swelling in the early days. Pain control plans may include appropriate local anaesthesia, tailored advice on analgesics, and clear instructions for cleaning, diet, and activity. Comfort also improves when expectations are realistic: some soreness, bruising, or temporary changes in speech can occur, and healing timelines vary by individual health factors and the complexity of the procedure. Follow-up reviews are important to catch pressure points, hygiene difficulties, or early signs of inflammation.
How are treatments tailored to individual needs?
Solutions tailored to individual dental needs usually begin with a structured assessment: gum condition, bite forces, remaining tooth structure, bone support, and aesthetic priorities. For some people, a fixed restoration may be appropriate; for others, staged treatment, gum therapy first, or alternative restorative options may be safer. Personal factors such as smoking status, diabetes control, clenching or grinding, and ability to maintain daily cleaning routines can influence the plan. A tailored approach should also include maintenance planning—how you will clean around the restoration, how often professional reviews are recommended, and what warning signs (bleeding, persistent soreness, loosening) should trigger an earlier check.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Modern restorative care tends to work best when it combines realistic goals with good diagnostics and a maintenance mindset. Digital planning and less invasive techniques can support comfort and predictability, but long-term success still relies on healthy gums, controlled bite forces, and consistent hygiene. Understanding the language used—such as “screwless” or “digital workflow”—helps you focus on practical questions about suitability, risks, retrieval for maintenance, and follow-up, which are central to making sense of today’s restorative choices.




